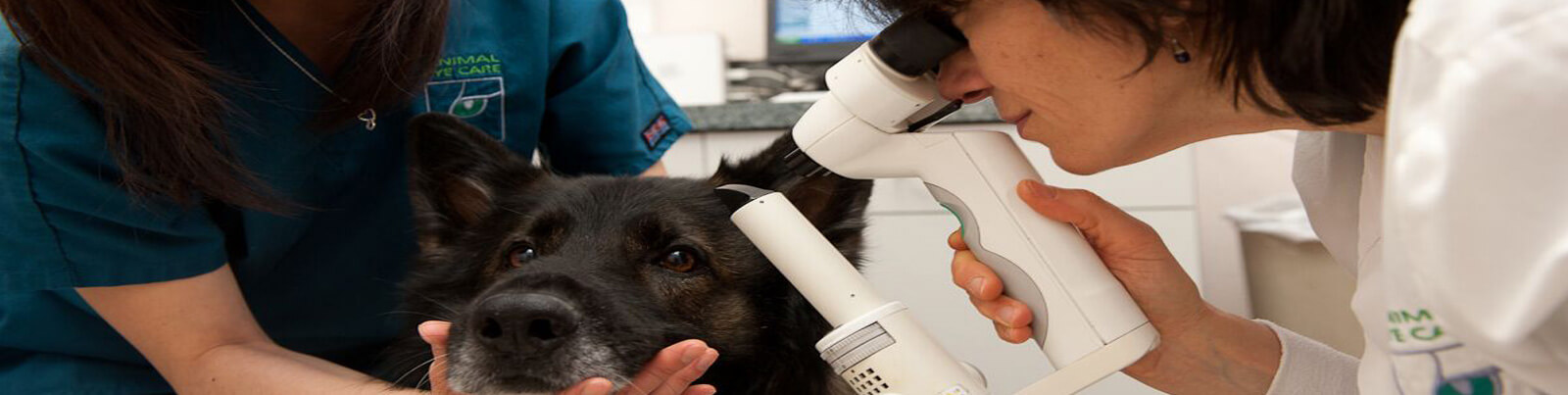
How Does My Pet’s Eye Exam Differ From My Own?
Many elements of an animal eye exam are very similar to those you experience when you visit your own ophthalmologist. A new patient eye exam at Animal Eye Care typically lasts anywhere from 45 minutes to an hour, beginning with a conversation with one of our registered veterinary technicians. They will obtain a thorough medical history – asking questions regarding medications, travel outside Northern California, other pets living in the household, etc.
Following the medical history intake, the technician will perform 3 different diagnostic tests:
- The first is the Schirmer Tear Test, which checks tear production and ensures that your pet is producing an adequate amount of tears.
- Next is IOP, or Intra-Ocular Pressure, during which the technician will numb the eyes with proparacaine drops and gently take the pressure of each eye. This step is in order to rule out glaucoma and any inflammation.
- Lastly, the technician will put fluorescein stain in each eye to check for any abnormalities or abrasions on the surface of the cornea. This will illuminate any ulcerations or abrasions when a black light is shined on the eyes.
After the 3 diagnostic tests are completed, the veterinary ophthalmologist will conduct a thorough front-to-back eye exam. They use special equipment to magnify internal structures of the eye, and allows the ophthalmologist to examine the eye for any abnormalities.
When handling energetic or nervous pets, we utilize different techniques that are unique to the pet’s needs. Sometimes wrapping the pet in a blanket or asking the pet owner to restrain their pet is helpful and allows the pet to feel more at ease. In some cases, we offer either oral or injectable sedatives to provide a more comfortable experience for the pet. Our staff go through comprehensive training to understand these methods and how they work to prevent and alleviate fear, anxiety, and stress in pets.
Here’s a closer look at each part of these examinations:
Schirmer Tear Test
In order to measure tear production, paper tear test strips are placed on the outer corners of each of your pet’s eyes between the lower eyelid and cornea for one minute. Evaluation then determines whether or not the pet is producing a healthy amount of tears. Detection of low tear production allows early diagnosis of KCS or “dry eye.”
Tonometry
After administering numbing eye drops, a digital tonometer is gently touched to the patient’s cornea to determine pressure inside the eye. High pressure could be indicative of glaucoma, while low pressure may be the result of inflammation in the eye.
Fluorescein Stain
An orange, water-soluble dye is applied to the surface of each of your pet’s eyes. This dye displays an intense green-fluorescent color when viewed under a cobalt blue light. A normal cornea without any scratches or ulcerations will not retain the dye. Any break on the surface of the eye will allow the dye to become absorbed by the corneal scratch or ulcer and will appear bright green. The fluorescein stain test is also used to evaluate the flow of tears through the nasolacrimal duct (tear ducts) to the nostrils.
Biomicroscopy
A hand-held microscope called a slit-lamp allows the ophthalmologist to view lesions or abnormalities within the eyelids, the surface of the eyeball, and the inside structures of the eye, such as the lens and anterior vitreous – the transparent gel that occupies more than two-thirds of the globe. By using the intricate lenses of the slit-lamp, the ophthalmologist can also examine the posterior segment of the eye, including the retina. The retina sends information to the brain through the optic nerve, enabling your pet to see. The great magnification of the slit-lamp allows the ophthalmologist to find small foreign bodies, misplaced eyelashes and microscopic signs of ocular disease.
Direct Ophthalmoscopy
The direct ophthalmoscope gives a largely magnified view of the eye as a whole. Performing distant direct ophthalmoscopy is an excellent tool to evaluate even the slightest differences in pupil size.
Indirect Ophthalmoscopy
Using a headset and hand lens allows the ophthalmologist to examine the structures in the back of the eye, including the vitreous humor, retina, and optic nerve.